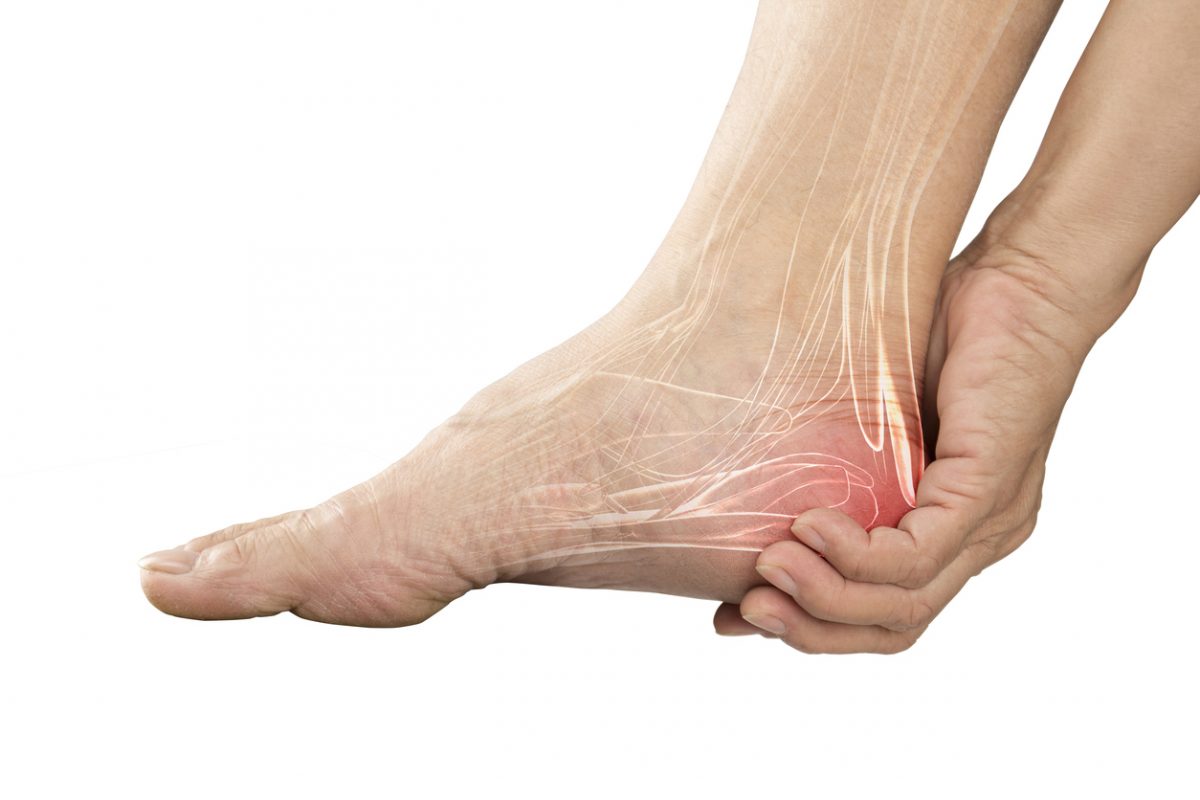
Could Your Foot Pain Be Caused by a Problem With Your Back?
While it doesn’t seem like there should be such a connection, considering how sensitive and large the back is, foot pain can in fact be related to your back. It is not uncommon to have pain in the legs or feet without any significant lower back pain, yet the problem is still originating in the lumbar region of the lower back. Blame the funny way our nerves work sometimes, sending signals all over the place.
You might blame that foot pain on the sciatic nerve
If a nerve root in the lower back – or lumbar area of the spine – is irritated or compressed, this lower back condition can cause pain to radiate along the sciatic nerve all the way to the patient’s foot.
The sciatic nerve is a large nerve that begins near the base of the spine, extending downward through the lower extremities, traveling through the hips, buttocks, and legs, before coming to an end in the feet near the toes.
Symptoms of Sciatica
As we age, the lumbar spine begins to deteriorate and weaken. This can impact the sciatic nerve, and lead to symptoms of sciatica, including:
· Pain
· Numbness
· Tingling
· Weakness
· Slower reflexes
· Muscle spasms
The sciatic nerve is very important, as it sends sensory and motor information to much of the lower body. The sciatic nerve is what sends the commands which allow for basic movement, such as walking and sitting. When this nerve becomes constricted, inflamed, or compressed in the lumbar spine, often due to degenerative spine conditions that develop in the lower back, the set of symptoms is known as “sciatica”.
Conditions that can cause sciatica
There are several degenerative spine conditions which can lead to the impingement or compression of the sciatic nerve, including:
· Lumbar degenerative disc disease
· Facet disease
· Lumbar spinal stenosis
· Lumber herniated disc
· Foraminal stenosis
· Isthmic spondylolisthesis
· Osteoarthritis
Treatment Options
Once your doctor diagnoses the cause of your pain as sciatica, a series of conservative treatment options may be recommended. Often, a combination of these treatments can sufficiently manage the problem. These may include:
· Activity modification
· Oral nonsteroidal anti-inflammatory medications
· Epidural injections
· Low-impact exercises
· Stretching techniques
· Physical therapy
When these conservative approaches to managing sciatica fail, it may be necessary to consider addressing the underlying cause with surgery.
If you are experiencing pain in your foot, or lower extremities, contact the Tucson Orthopaedic Instituteat one of their several area locations. You can schedule an appointment online, to be examined by one of their highly qualified, board-certified orthopedic surgeons. At Tucson Orthopaedic Institute, there are many non-invasive treatment options for diagnosing and treating sciatica, and we will work with you every step of the way until your pain subsides.