We all know that regular exercise is an essential part of a healthy lifestyle. Exercise makes you look and feel good, promoting greater muscle strength, endurance, flexibility, weight control, and cardiovascular fitness.
However, too much of a good thing can lead to an injury that can sideline you from the activities you enjoy. You don’t have to be a competitive athlete to have a sports injury, which is simply an injury that occurs during sports or exercise. A sports injury can happen to anyone at any age; although they are more common as we grow older, and more often occur among women, due to differences in body structure. 
Sports injuries can involve any part of the body, but generally refer to an injury that involves the muscles, bones or a soft tissue, such as cartilage in the knee. These injuries usually occur from improper training or conditioning, insufficient warm-up and stretching before an activity, using the wrong equipment, or doing too much, too fast.
Sports injuries fall into two primary categories: acute and chronic. An acute injury involves a specific event that causes trauma, such as a fall or a collision. A chronic injury occurs with repetitive motions and excessive cumulative strain on the musculoskeletal system.
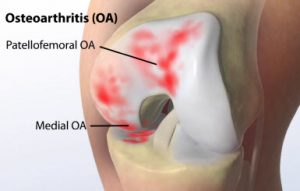
Prompt treatment of both acute and chronic injuries is important in avoiding further injury. Injuries left untreated or not allowed to fully heal can lead to recurrent injuries, or develop into more serious long-term problems, such as osteoarthritis.
It’s important to distinguish muscle soreness from injury in deciding whether to seek medical help. The traditional credo of rest, ice, compression and elevation is effective for home care. However, if you’ve tried these steps after injury and pain and swelling do not improve, contact your doctor. Signs that your injury needs medical attention include worsening or persistent pain, swelling, numbness or abnormal appearance.
If you suspect you’ve sustained a sports injury, a good place to start is with your primary care provider. He or she may consult with a sports medicine specialist to facilitate with diagnosis and treatment. Depending on your injury, you may receive care from an orthopedic doctor or a rehabilitative therapist. An orthopedic doctor specializes in the diagnosis and treatment of the musculoskeletal system; a physical therapist works in partnership with your sports medicine doctor to rehabilitate your injury and return you to athletics safely.
Treating a sports injury is a gradual process. Improving range of motion as pain resolves is the first step to help speed healing. Rehabilitation is based on a progression of activities to help build flexibility, endurance, and strength, as well as proper balance and body mechanics. In addition to exercise, your therapy may include various modalities including but not limited to: electrostimulation (mild electrical current to reduce pain and swelling and increase muscle strength), cryotherapy (ice packs to limit blood flow to injured tissues), heat, ultrasound and massage.
Arthroscopic surgery, an operation that employs small incisions to diagnose and fix joint abnormalities, has greatly enhanced physicians’ ability to repair athletic injuries without invasive surgery, resulting in less trauma and downtime for the patient. Other new advances being studied include tissue engineering, in which a patient’s own healthy cartilage or cells are transplanted to an injured area to speed healing.
Benefits of rehabilitative therapy include restoration of function, less pain, improved range of motion, a more timely and safe return to sports, and recreational activities. Other benefits include an improved a sense of wellbeing, cardiovascular fitness, strength, flexibility, balance, and muscle coordination.
Play It Safe
Practicing smart sports and exercise habits can prevent an injury on the front end. The National Institute of Arthritis and Musculoskeletal and Skin Diseases recommends the following techniques to avoid injury:
- When doing knee bends, don’t bend your knees more than halfway.
- Don’t twist your knees when you stretch; keep your feet flat.
- When jumping, land with your knees bent.
- Do warm-up exercises before playing any sport.
- Always stretch before you play or exercise.
- Cool down after hard sports or workouts.
- Wear shoes that fit properly, are stable and absorb shock.
- Exercise on the soft surfaces; don’t run on asphalt or concrete.
- Run on flat surfaces.
- Don’t be a weekend warrior, i.e., engaging in a week’s worth of activity in a day or two.
- Learn to do your sport right. Use proper form to reduce your risk of overuse injuries.
- Use the appropriate safety gear for the sport you are playing.
- Build up your exercise level gradually. Know your body’s limits.
Sports Injuries
Part of treating a sports injury is being able to explain symptoms to your doctor. Here is a list of the most common types of sports injuries (from the National Institute of Arthritis and Musculoskeletal and Skin Diseases)
Sprain: A stretch of tear of a ligament, the band of connective tissues that joins the end of one bone with another
Symptoms: Tenderness or pain, bruising, swelling, inability to move a limb or joint, instability
Strain: A twist, pull or tear to a muscle or tendon, which is tissue that connects muscle to bone
Symptoms: Pain, muscle spasm and loss of strength
Dislocated joint: When two bones that come together to form a joint become separated, through impact sports, excessive stretching or falling
Symptoms: Severe pain, joint is visibly altered and moves unnaturally, or cannot be bent or straightened properly
Fracture: A break in the bone that can occur from either a quick, one-time injury (acute fracture) or from repeated stress to the bone over time (stress fracture)
Symptoms: Pain at the site and inability to bear weight (acute) or pain at the site that worsens with weight-bearing activity (stress)
Article written by William Prickett, MD, Tucson Orthopaedic Institute Sports Medicine Surgeon
Published on TusconLocalMedia.com, Wednesday, March 13, 2013


 I travelled with 50 team members that consisted of six orthopaedic surgeons and four anesthesiologists, as well as scrub techs, physician assistants, nurses, physical therapists, and other volunteers. To get there, the physicians paid their own travel expenses, while the rest of the group was supported by contributions and donations made to Operation Walk.
I travelled with 50 team members that consisted of six orthopaedic surgeons and four anesthesiologists, as well as scrub techs, physician assistants, nurses, physical therapists, and other volunteers. To get there, the physicians paid their own travel expenses, while the rest of the group was supported by contributions and donations made to Operation Walk.
 What is the advantage of a partial knee replacement?
What is the advantage of a partial knee replacement? 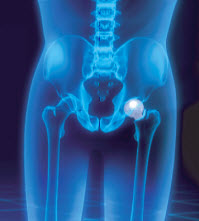







 As part of the program, the surgeons from Tucson Orthopaedic Institute, and anesthesiologists from Old Pueblo Anesthesia, will donate their time and expertise. Hospitalists will be volunteering time to care for patients after their surgery. Tucson Medical Center is donating the space and necessary prescription medications. Stryker Orthopedics is providing the joints, and Gentiva will provide free home health services to assist these patients during their recovery.
As part of the program, the surgeons from Tucson Orthopaedic Institute, and anesthesiologists from Old Pueblo Anesthesia, will donate their time and expertise. Hospitalists will be volunteering time to care for patients after their surgery. Tucson Medical Center is donating the space and necessary prescription medications. Stryker Orthopedics is providing the joints, and Gentiva will provide free home health services to assist these patients during their recovery.
 Dr. Cohen joined the group this year to help with the mission and to support Dr. Piedrahita’s worthy cause. The team laughed and also cried, and enjoyed each other’s company. The experience left them all feeling enriched and thankful for the chance to give back.
Dr. Cohen joined the group this year to help with the mission and to support Dr. Piedrahita’s worthy cause. The team laughed and also cried, and enjoyed each other’s company. The experience left them all feeling enriched and thankful for the chance to give back.